Today, October 20, 2021, marks World Osteoporosis Day (WOD) – an annual event championed by the International Osteoporosis Foundation (IOF), dedicated to raising global awareness of the urgent need for prevention, diagnosis and treatment of osteoporosis and related musculoskeletal diseases.
Aligned with the IOF’s global efforts to engage healthcare professionals, policy makers, patients, and the public at large to prioritise bone health and fracture prevention on the global health stage, throughout the year-long annual WOD campaign, the Asia Pacific Fragility Fracture Alliance (APFFA) is similarly dedicated to delivering effective osteoporosis care, fewer fractures, and better outcomes for people living with osteoporosis in the Asia Pacific.
Osteoporosis care has been significantly compromised by the global pandemic. The past two years have been tainted by treatment delays, and an excessive, sedentary indoor lifestyle.
According to IOF President, Professor Cyrus Cooper, UK, the pandemic’s ongoing toll on bone health and the timely delivery of osteoporosis assessment and care is of global concern.
“Given this backdrop, it is more important than ever to be proactive on behalf of bone health.
“Osteoporosis-related fractures are a major cause of pain, disability, and loss of independence in older adults. Such life-changing injuries can be prevented with life-long attention to bone health, and early diagnosis and appropriate treatment for those at risk,” said Prof Cooper.
Chair of IOF Asia-Pacific and South Africa Regional Advisory Council, and co-Chair of the APFFA Joint Steering Committee, Dato’ Dr. Joon-Kiong Lee, Malaysia, echoes the IOF President’s sentiments, also calling for renewed attention and prioritisation of bone health today.
“Globally, osteoporosis accounts for nearly nine million fractures each year,1 with more than 200 million living with osteoporosis world-wide.2
“In the Asia Pacific alone, the world’s fastest ageing population, mounting urbanisation, and our subsequent increase in sedentary lifestyles3 will contribute to the 319 million people aged over 50 years who are anticipated to be at heightened risk of osteoporotic fracture over the ensuing 20 years.4 By 2050, more than half the world’s hip fractures are expected to occur in our region,”5 Dato’ Dr. Lee said.
This year’s WOD under the theme ‘Take action for bone health’, calls on all stakeholders to take responsibility for bone health in the global fight against osteoporosis.
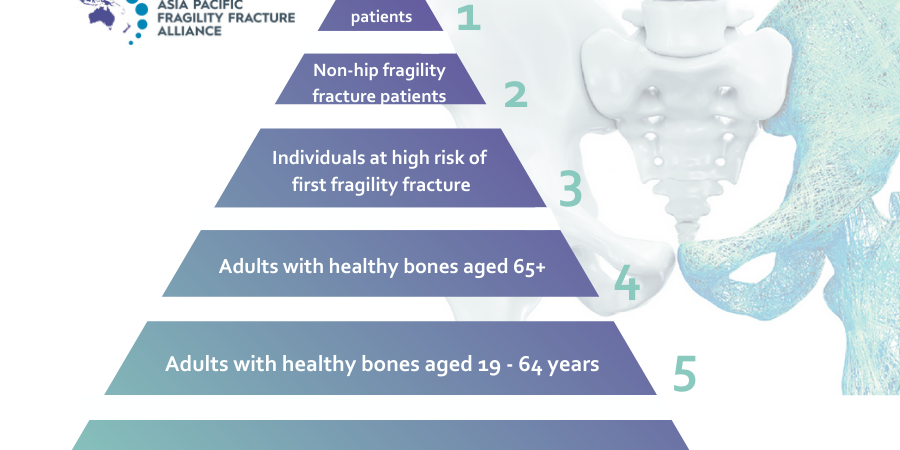
Vice-Superintendent of the National Taiwan University Hospital, and Co-Chair of the APFFA Joint Steering Committee, Professor Derrick Chan, Taiwan, said patients are encouraged to take the following five active steps to improve their own bone health:
- Maintaining adequate levels of exercise, including weight-bearing and muscle strengthening routines to help preserve bone and muscle mass.
- Participating in lifestyles that encourage regular exposure to sunlight and adequate intake of vitamin D rich foods, and importantly, seeking advice from a doctor on Vitamin D supplementation to promote healthy bones.
- Learning about the risk factors of osteoporosis by taking the IOF Osteoporosis Risk Check survey, and requesting a fracture risk assessment, if found to be at heightened risk of fracture.
- Ensuring diligence and adherence to osteoporosis treatment regimes for those prescribed with osteoporosis medications.
- Establishing a safe home environment to minimise the risk of falls.
The message for policy makers and health authorities this WOD is to advocate for renewed attention to the burden of osteoporosis, shift perceptions, and call for change.
“World Osteoporosis Day is a fitting occasion to remind all healthcare authorities that there is a proven way to stop this devastating and costly cycle of recurring fractures,” said Prof Cooper.
“All fracture patients must be screened and treated through a post-fracture care model, such as a Fracture Liaison Service (FLS), which has been shown to reduce re-fracture rates and mortality, and ultimately reduce the burden of fractures on healthcare systems.”
APFFA promotes the widespread implementation of the FLS model of care to reliably deliver secondary fracture prevention, and ensure the best transition of care from hospital to community.
FLSs are designed to encourage the assessment and management of osteoporosis and falls risk.6
A growing global body of evidence supports implementation of a FLS7 which have been found to improve the:
- Identification of all fractures;
- Percentage of anti-osteoporosis medication recommendations; and
- Volume of patients who received (or were referred for) a falls assessment.8
The APFFA Education Directory – a curated collection of materials from the Asia Pacific region supporting education on osteoporosis and fracture prevention for a range of audiences – links to Making the Best of FLS – Key performance Indicators Webinar, comprising complimentary slides by Prof. Kassim Javaid and Prof. Serge Ferrari, that aim to improve understanding, and encourage implementation of, key performance indicators that drive quality improvement for FLSs, to realise the full potential of secondary fracture prevention.
IOF Chief Executive Officer, Dr Philippe Halbout, Switzerland, urges all health care authorities to implement post-fracture care coordination programmes in their hospitals.
“It’s an investment that pays off in terms of healthcare investment and, most importantly, by helping older adults remain healthy, active, and independent as they age.”
To learn more about APFFA and the organisation’s ongoing commitment to reducing the burden of osteoporosis in the Asia Pacific, visit https://apfracturealliance.org.
To learn more about WOD, visit www.worldosteoporosisday.org.