The Hip Fracture Registry (HFR) Toolbox
Developed by the APFFA Hip Fracture Registry Working Group, in collaboration with the Fragility Fracture Network (FFN) Hip Fracture Audit Special Interest Group
The world-first Hip Fracture Registry (HFR) Toolbox is a practical and informative resource that extracts key findings from existing national and regional hip fracture registries, to advocate for, and support clinicians, hospital administrators, healthcare systems and governments with, establishing a national registry in their respective countries.
The Toolbox:
- Explains the fundamental need for hip fracture registries;
- Features a practical guide on the various components involved in establishing a registry;
- Offers direction on stakeholder engagement and consolidation; advocating for change; planning and funding a registry; setting up a pilot registry; navigating governance and ethics approval and adopting a minimum common dataset (MCD); and
- Includes established registry case studies and other useful resources.
To learn more about the HFR Toolbox, download our HFR Toolbox Media kit here.

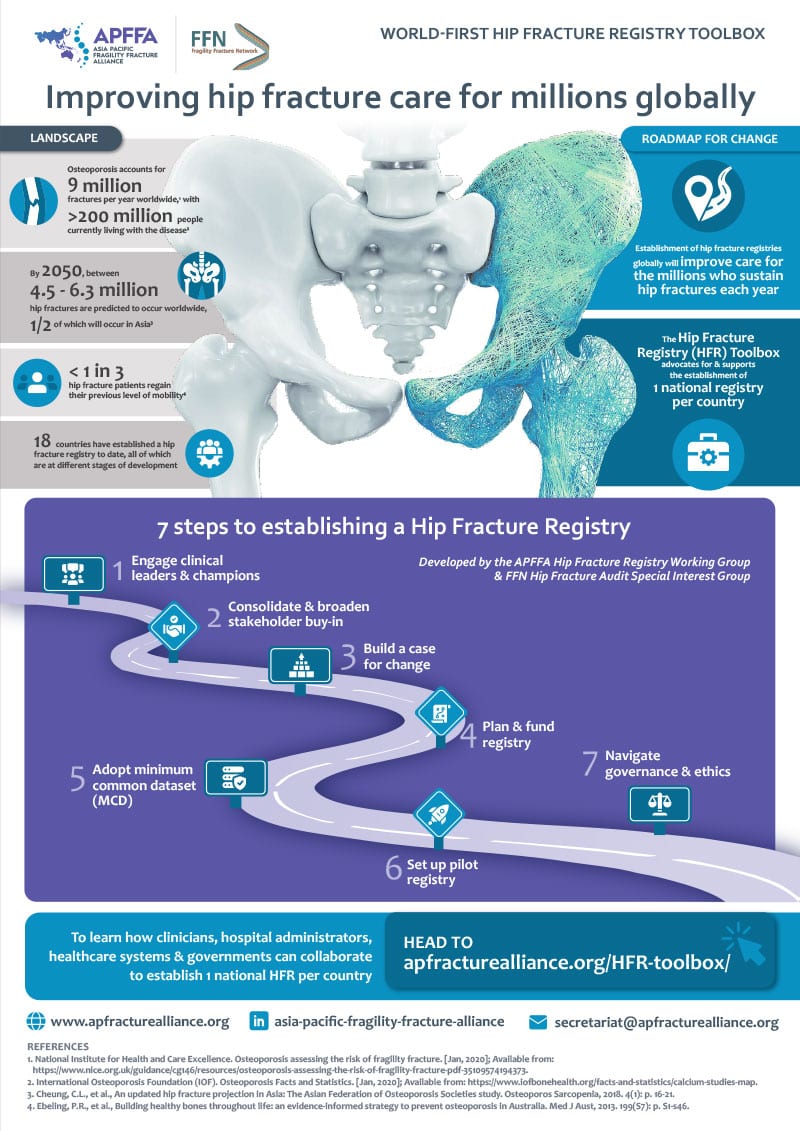
7 steps to establishing a HFR
- Engage clinical leaders and champions.
- Consolidate and broaden stakeholder buy-in.
- Build a case for change.
- Plan and fund a registry.
- Adopt a minimum common dataset (MCD)
(Download the FFN Minimum Common Dataset here). - Set up a pilot registry.
- Navigate governance and ethics.
Purpose of a HFR
- Registries for any health condition provide a mechanism to identify and investigate variations in the provision of patient care.
- Widescale implementation of HFR's globally can facilitate vast improvements in care for the millions of people who sustain a hip fracture each year.
- Given the exponential increase in both the incidence and costs associated with hip fractures to date, and those anticipated globally,1 HFR's act as an essential tool for clinicians, hospital administrators, healthcare systems and governments in the Asia Pacific region, and worldwide, to underpin quality improvement initiatives.
- Hospitals can utilise HFR's to benchmark their provision of care against best practice clinical standards for acute care, rehabilitation, and secondary fracture prevention.
- Furthermore, HFR's transform patient-level data into information that can equip and empower hospital teams to identify the key challenges to overcome within their respective institutions, develop solutions to these challenges, and therefore, strive for ongoing improvement in care.

The driver for change
- By 2050, 1-in-4 people in the Asia Pacific will be aged over 60. This portion of the population is expected to triple between 2010 and 2050, reaching close to 1.3 billion people.2
- Within the same timeframe, between 4.5 to 6.3 million hip fractures are predicted to occur worldwide, half of which will occur in Asia.3
- More than 1.1 million hip fractures were estimated to have occurred in China, Chinese Taipei, Hong Kong SAR, India, Japan, Malaysia, Singapore, South Korea and Thailand in 2018, incurring an estimated direct cost of USD 7.5 billion. This cost is projected to increase to almost USD 13 billion by 2050.4
- Even more concerningly, 1-in-4 patients who sustain a hip fracture die within a year, and less than half of those who survive, regain their previous level of function.5,6
- With adequate operational efficiency and funding, registries can improve healthcare, and are likely to prove significantly cost-effective.7
- Registries can contribute to government initiatives designed to manage rapidly aging populations, and can further help governments to promote the equitable provision of care.8
Download the
HFR Toolbox
Thank you for your interest in the HFR Toolbox. This Toolbox has been developed to help the user to navigate the various stages and complexities of establishing a national Hip Fracture Registry. The Toolbox arms the user with an overview of key lessons learned in the establishment of hip fracture registries to date, and practical tools to support registry development.
Both APFFA and FFN highly recommend that each country has 1 national Hip Fracture Registry. The FFN Hip Fracture Special Audit Interest Group and the FFN Regionalisation Committee provide networking opportunities for national registry champions to share their experiences and learn from each other.
We strongly advise all clinicians, hospital administrators, healthcare systems and government representatives to collaborate and contribute to 1 national registry in their respective country.
HFR Toolbox Media Kit
If you wish to be informed about new resources relating to the APFFA-FFN HFR Toolbox, please click below.
- Baker, P.N., et al., Evolution of the hip fracture population: time to consider the future? A retrospective observational analysis. BMJ Open, 2014. 4(4): p. e004405.
- United Nation Population Fund (UNFPA) Asia & the Pacific. Ageing. [cited 2021 May]; Available from: https://asiapacific.unfpa.org/en/node/15208.
- Cheung, C.L., et al., An updated hip fracture projection in Asia: The Asian Federation of Osteoporosis Societies study. Osteoporos Sarcopenia, 2018. 4(1): p. 16-21.
- Ebeling, P., et al., Secondary prevention of fragility fractures in Asia Pacific: an educational initiative. Osteoporosis International, 2019.
- National Osteoporosis Foundation, NOF's Clinician's Guide to Prevention and Treatment of Osteoporosis.
- Australian Institute of Health and Welfare. Musculoskeletal fact sheet. Osteoporosis. [Jan, 2020]; Available from: https://www.aihw.gov.au/getmedia/61866386-568b-41fa-93e4-090ad201ab2b/phe187-osteoporosis-factsheet.pdf.aspx
- Australian Commission on Safety and Quality in Health Care, Economic evaluation of clinical quality registries. 2016.
- Australian Government, National Clinical Quality Registry and Virtual Registry Strategy - A National Strategy for Clinical Quality Registries and Virtual Registries 2020-2030. 2020.