Throughout 2020, the Australian & New Zealand Hip Fracture Registry (ANZHFR) produced an informative, 16-part online lecture series designed to share best practice in relation to the treatment and management of hip fractures, and to offer clinicians potential solutions to common problems. The series is available on the ANZHFR Training and Education YouTube channel – a selection of which has recently been added to our APFFA Education Directory.
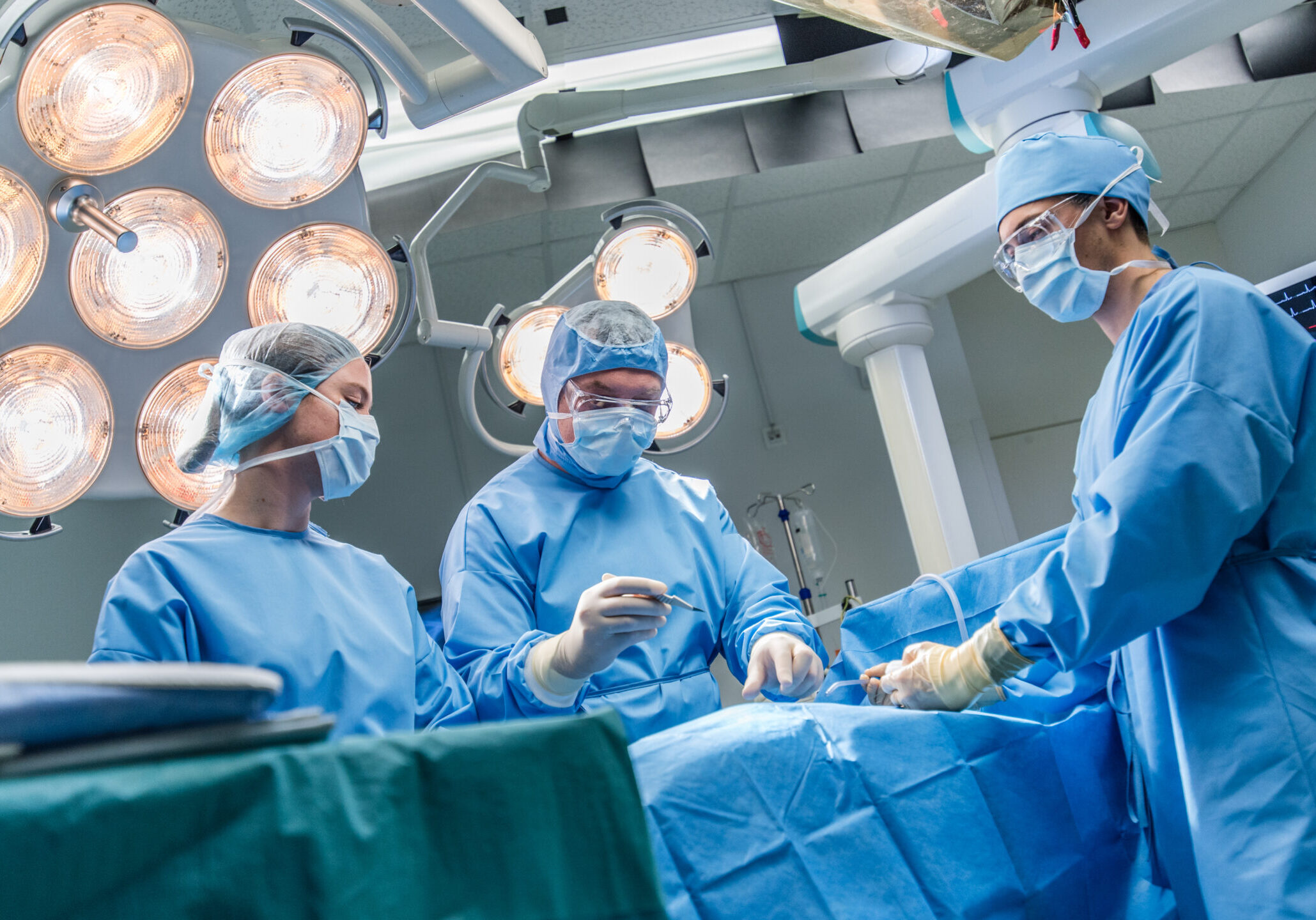
In the lecture published on August 10, 2020, Australian APFFA Joint Steering Committee (JSC) members, Geriatrician and Medical Director, Fiona Stanley Hospital, Dr Hannah Seymour, and ANZHFR Co-Chair, Professor Jacqui Close, discuss when not to operate on hip fracture patients nearing the end of their lives, and when palliation should be considered, instead.
The question of when not to operate, and when to palliate instead, is a highly contested topic that troubles many clinicians worldwide.
In her discussion, Dr Seymour anecdotally reflects on the patient cohort who would not benefit from hip fracture surgery. Each year, Dr Seymour and her colleagues at Fiona Stanley Hospital care for approximately 500 hip fracture patients, 15 of whom die during acute care (based on an approximate 3 per cent acute mortality rate).
“It constantly surprises me who survives an operation, and how much in our heads we overestimate mortality perioperatively,” said Dr Seymour.
“The group of patients selected for palliation is actually very small. In our group of 500 hip fracture patients each year, we choose not to operate on approximately 5 patients. I recall one such patient who had very severe lung disease, died within 24 hours of hospital admission, and was clearly too unwell for surgery.
“Another example was a patient with end stage renal failure, who was struggling to manage dialysis because of his dementia. Following a fall, he was admitted with a hip fracture, and also presented with a brain injury and a large intracerebral haemorrhage,” Dr Seymour said.
In her lecture, Dr Seymour provides advice on how she strives to ensure the delivery of effective palliative care when the decision not to operate has been made, explaining:
- For the very small group of patients, who are on a rapid downward trajectory, then standard non-operative palliative care is generally the approach. This includes subcutaneous morphine and palliation to ease distress and address any particular needs.
- For the group of patients in between, it is important to discuss the best approach with a multidisciplinary team, considering the patient’s overall operative risk.
Shared decision making is based on determining the patient’s care goals, and safeguarding patients who are unlikely to benefit from operative treatment, particularly if they are in the palliative or terminal phase of life. A shared decision making approach with the medical team, the patient and their family, is pivotal to this decision making process.
“The more we do this, the more we grow comfortable with having shared decision making discussions with patients and their families, about the reasons to operate – namely, to improve comfort and quality of life.
“By choosing to operate, patients are given the certainty that they are going to have a surgery, and that their pain and condition is likely to improve,” said Dr Seymour.
In Australia, the shared care approach is documented in the Hip Fracture Care Clinical Care Standard (September 2016), a resource developed by the Australian Commission on Safety and Quality in Health Care, which provides guidance to Australian consumers, clinicians and health services alike, on delivering appropriate care to those who have sustained a hip fracture.
In their lecture, Dr Seymour and Prof Close explain that even with a wealth of clinical experience, it is important to not debate the decision too much, given this extends the preoperative time, and in some cases, people actually do worse as a result. Being comfortable with having these difficult discussions is something that comes with time.
“We need to constantly remind ourselves and our teams of the data available to us. Using your own local data to have that discussion is really important. Looking at your own local mortality rate and reviewing the cases of those who have died, helps you learn more about which groups of patients you should consider not operating on, more often,” Dr Seymour said.
Prof Close confirmed that Dr Seymour’s anecdotal experience together with data collected on hip fracture patients at the end of their lives, is consistent with data collected by the ANZHFR.
“Your data is very similar to what we see in the ANZHFR, whereby the vast majority of hip fracture patients will still undergo surgery. In the small number of patients where surgery doesn’t change their outcome, so long as we have good palliative care to support us, then hopefully their outcome is a dignified exit from this world,” said Prof Close.
In summary, it is important to consider all options available, to weigh up the various risks and benefits, and to then pursue a shared care approach involving the medical care team, and the patient and their family.
To learn more about the latest updates in hip fracture care, subscribe to the ANZHFR Education and Training YouTube Channel. To watch the full lecture, click here.