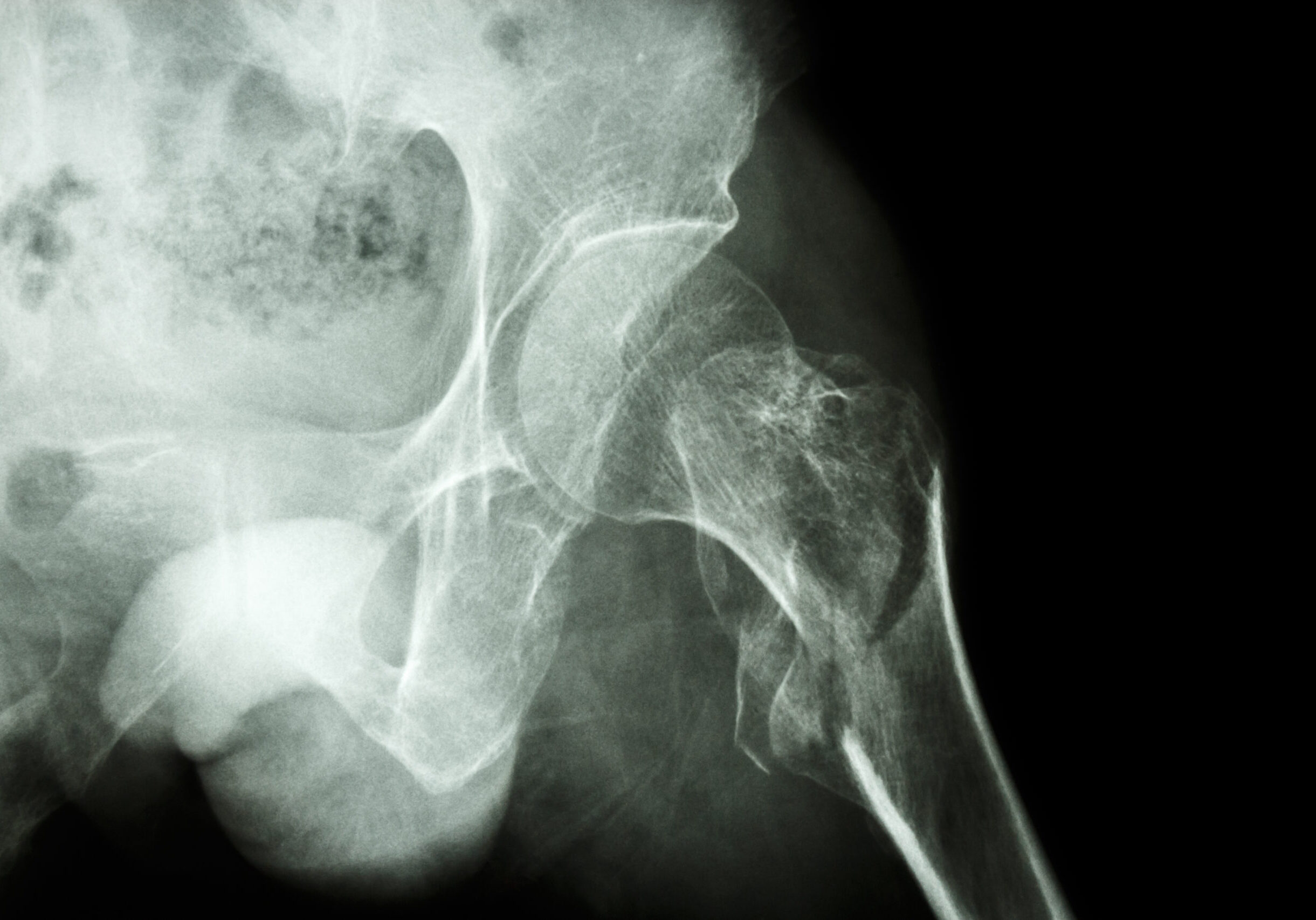
One-in-10 hip fracture surgeries are performed to manage a contralateral hip fracture in those aged over 60 years who have sustained an initial hip fracture, according to a recent retrospective review published in the Irish Medical Journal. Concerningly, nearly 50 per cent of the second hip fractures occur within three years of the first, most commonly during the first year of the initial injury.
These findings support the provision of Fracture Liaison Services (FLS) – multi-disciplinary, coordinator-based, secondary fracture prevention services implemented by health care systems to enhance communication between healthcare providers and fragility fracture patients. Furthermore, they reinforce the importance of early initiation of bone protecting medications following an initial fracture, and interventions to prevent falls, to help reduce the risk of secondary fractures.
Hip fractures are among the most common hospital presentations for the older population, noting approximately two million hip fractures occur globally each year – a figure set to rise up to four-fold by 2050.
Hip fractures among older adults compromise mobility, independence and quality of life. Less than one-in-three hip fracture patients regain their pre-fracture level of mobility, and may experience a reduction in overall functional status, social independence, mobility, and an increase in depressive symptoms. Those who sustain a second contralateral hip fracture are less likely to be discharged home, and more likely to be discharged to a nursing home. Moreover, hip fractures impose a high economic toll on hospitals, further emphasising the need for secondary prevention among this patient cohort.
Despite substantial improvements made to hip fracture care over the past 30 years, as the world’s global ageing population continues to rise, a significant increase in the prevalence of fractures is expected.
According to the International Osteoporosis Foundation (IOF) global ‘Capture the Fracture® program, which advocates the use of FLS worldwide:
- The first fracture a patient sustains is often not interpreted as a warning sign for future fractures; and
- There is a “care gap”, given 80 per cent of those who sustain a fragility fracture are not offered screening and/or a treatment regimen for osteoporosis.
Secondary fracture prevention is possible, and of substantial benefit. Importantly however, successful fracture prevention measures depend not only on investigation and initiation of treatment, but on maintenance of treatment – adherence and compliance.
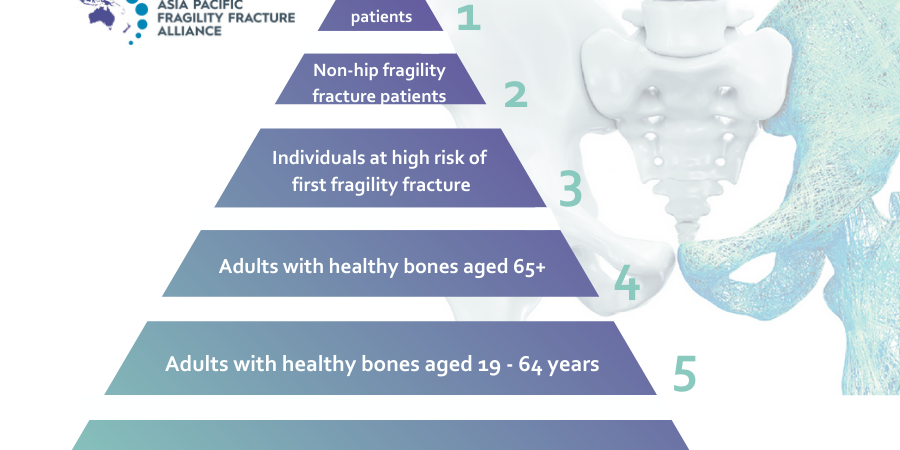
APFFA is an alliance of seven global and regional member organisations (including the IOF), from the geriatrics, orthopaedics, osteoporosis and rehabilitation sectors, committed to secondary prevention of fragility fractures, throughout the Asia Pacific region.
APFFA’s primary purpose is to drive policy change, improve awareness and change political and professional mindsets to facilitate optimal fragility fracture management. Our mission is to promote multidisciplinary collaboration and change policy to facilitate best practice in the acute care, rehabilitation and secondary prevention of fragility fractures.