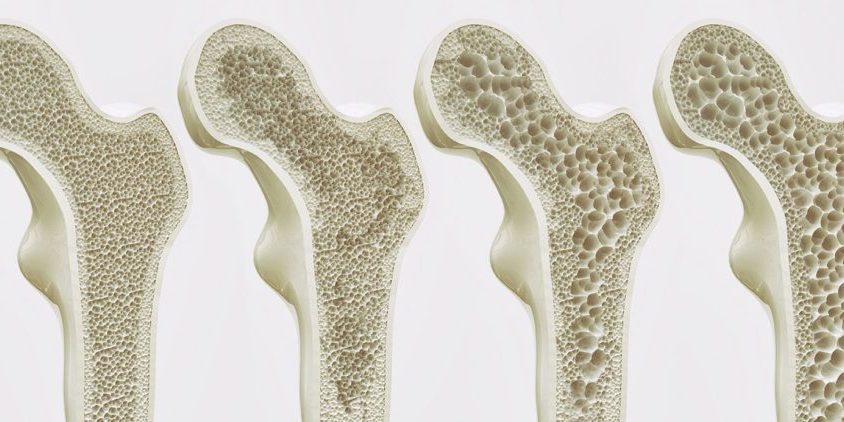
Less than one-in-four Malaysians able to walk independently post-hip fracture
Epidemiological data has projected an unprecedented increase in the incidence of hip fractures worldwide over the ensuing decades. Predictions suggest that by 2050, there will be up to six million hip fractures sustained globally each year, half of which will be borne by the Asian Pacific region.
According to a recent narrative review published in the Malaysian Orthopaedic Journal, Malaysia is expected to experience one of the highest rates of hip fracture in the region. In 2010, only five per cent of older people were aged 65 years and over. However, by 2040, this figure is anticipated to increase exponentially, to more than 14 per cent, equating to six million people. Most of this population will also be living longer – the average life expectancy is projected to increase from 74 years of age, to 81 years by 2050.
Warning of the devastating future toll that hip fractures are set to incur on health services in Malaysia, and indeed, upon the rest of the world, local and international experts alike are calling for urgent action to address this mounting health challenge.
Hip fractures, which represent the most frequent fragility fracture sustained by older populations, are often indicative of underlying osteoporosis, with falls identified as the most common aetiology. Hip fractures are associated with increased morbidity, disability and mortality. Management of hip fractures consequently consumes substantial healthcare resources, including inpatient beds, surgical intervention, and ongoing support for daily living upon hospital discharge.
Analysis of the Malaysian population who have sustained a fracture six months post- discharge, revealed less than one-in-four were able to walk independently, 14 per cent were immobile, the remainder required a walking aid, while nearly 60 per cent were dependent upon others for fulfilling activities of daily living.
Orthopaedic Surgeon and APFFA co-Chair, Dato’ Dr. Joon-Kiong Lee, Malaysia, explains that 25 per cent of those who have sustained a hip fracture in Malaysia report having experienced at least one previous fall; 13 per cent report having endured a fragility fracture; while 5 per cent cite having already sustained a hip fracture.
“What’s most concerning is that despite these individuals being at heightened risk of fragility fracture, only 12 per cent of the cohort were on bone health optimising medications.
“Furthermore, less than one-in-five were operated on within the recommended 48-hour timeframe from hospital admission. The median timeframe for surgical intervention was five days,” said Dr Lee.
“While falls and osteoporosis are preventable, or at the very least, modifiable in Malaysia, concerningly, neither are routinely addressed in hip fracture patients.”
Yet despite this concerning data from multiple clinical studies reinforcing the need for prompt action in Malaysia, osteoporosis, fragility fractures, and musculoskeletal health remains absent from any of Malaysia’s national health priorities.
Furthermore, while the international osteoporosis community has identified a highly effective model of care to both optimise and prioritise bone health – Fracture Liaison Services (FLS) – widespread implementation of FLSs is yet to be achieved in Malaysia. FLSs are supported by robust evidence and have been shown to reduce subsequent fractures and mortality by up to 50 per cent, and 35 per cent, respectively. Currently there are only three FLSs in Malaysia mapped under the IOF Capture the Fracture World Map, two of which are based in Kuala Lumpur, and one in Selangor. The Fragility Fracture Network Malaysia (FFNM) has however commenced efforts to establish a national FLS Framework, which is expected to be launched by third quarter of 2021.
Other effective models of care do however, exist. Diminished medical complications, reduced hospital mortality, time to surgery, and minimised functional deterioration have been demonstrated by an orthogeriatric approach to management of hip fracture patients, whereby patient care is concurrently managed by an orthopaedic surgeon and a geriatrician-led medical team. Currently three hospitals in Kuala Lumpur deliver orthogeriatric care.
“Key action items for Malaysia include widespread implementation of FLSs, and the need to address the current literature gap around hip fracture care,” Dr Lee said.
“Although efficacy of the wide-scale application of the collaborative orthogeriatric model of care, consistent with the standard of care in international hip fracture guidelines, is yet to be demonstrated in Malaysia, there is no reason to believe this will not be the case, given patient characteristics and issues are similar to what has been reported in other countries and regions.
“Significant recent efforts have been made by three leading osteoporosis and fragility fracture societies – Osteoporosis Awareness Society of Kuala Lumpur and Selangor (OASKLS), Fragility Fracture Network Malaysia (FFNM), and the Malaysian Osteoporosis Society, partnering to form the collaborative national alliance, Bone Health Alliance Malaysia (BHAM),” said Dr Lee.
The pioneering alliance aims to:
- Improve bone health education among local communities;
- Correct the misconception that osteoporosis is unpreventable;
- Organise meaningful stakeholder engagement; and
- Enhance osteoporosis treatment and diagnosis to improve patient outcomes.
Further, on a regional scale, APFFA, a multi-stakeholder alliance which aims to promote multidisciplinary collaborations and change policy to facilitate best practice in the acute care, rehabilitation and secondary fracture prevention of fragility fractures, is striving to achieve the prioritisation of bone health in Malaysia, and the greater Asia Pacific region.